How the U.S. Pandemic Response Went Wrong–and What Went Right–During a Year of COVID
When the World Health Organization first called COVID-19 a pandemic on March 11, 2020, few people had any idea what the world was in for. The progression was swift: borders clamped shut, authorities issued stay-at-home orders, and public life ground to a near halt. Most of the world had no experience dealing with an infectious disease outbreak of this scale. The previously unknown virus, now called SARS-CoV-2, could spread through the air, often before (or, in some cases, possibly without ever) causing any symptoms. COVID—though mild for many people—struck down elderly and more vulnerable individuals (and occasionally very healthy ones) with a vengeance, launching a wave of fear, suffering and death unlike any in recent memory.
“In the beginning, when this started a year ago, we knew that it was spreading. And we knew that it also was lethal in some percentage of people,” says Stanley Perlman, a virologist at the University of Iowa, who is an expert on coronaviruses, a group that includes SARS-CoV-2. “But I don’t think we had a full appreciation about how bad it was.”
Among the biggest shocks was that the U.S. fared worse than most other countries, with more than 29 million cases and nearly 530,000 deaths as of this writing. “We absolutely can’t say that we had the most robust response to the pandemic, up till this point, because we have had a higher death rate per capita than so many other places,” says Monica Gandhi, a professor of medicine at the University of California, San Francisco.
As the country raced to react to this new and terrifying scourge, mistakes were made that together cost hundreds of thousands of lives. Yet the tireless efforts of health care workers, along with an unprecedented vaccine push, have saved countless others. Scientific American interviewed scientists and public health experts about the biggest mistakes in the U.S.’s response, some of the key successes and the lingering questions that still need to be answered.
What Went Wrong
Downplaying the danger and sidelining experts. During the pandemic’s crucial early days and weeks, then president Donald Trump and other authority figures actively minimized the virus’s threat. Trump dismissed it as no worse than the flu and said the pandemic would be over by Easter.
“One thing that shouldn’t have been done is people downplaying the infection,” Perlman says. “That was a real big problem, because if you let the pandemic get out of control and don’t take it seriously, it gets worse.” The U.S. Centers for Disease Control and Prevention initially told the media that the threat to the American public was low. When a CDC spokesperson acknowledged in late February that disruptions to daily life could be “severe,” the agency was quickly sidelined—and Trump himself became the government’s main conduit for COVID updates through his daily briefings. “The Trump administration really tightly controlled what [the CDC] could put out,” says Angela Rasmussen, a virologist at the Georgetown University Center for Global Health Science and Security. This muzzling of the CDC and top government health experts made it hard for them to communicate accurate and lifesaving scientific information to the public. Under President Joe Biden’s administration, government science agencies and health officials have been given renewed respect and independence. But rebuilding public trust in these authorities will still take time.
Slow and flawed testing. The CDC developed its own test for the virus rather than employing a German-developed one used by the World Health Organization. But the CDC test was flawed, causing a deadly delay while scientists worked out the problem. The agency was not designed to produce tests at the scale needed to spot the infections as they silently spread through the population. Meanwhile the Food and Drug Administration was slow to approve tests made by private companies, says Caitlin Rivers, an epidemiologist at the Johns Hopkins Center for Health Security. She also says the earliest criteria for getting a test were too stringent—one often had to have been hospitalized with severe symptoms and have recently traveled to a “high-risk” area. As a result of these hurdles, the virus spread undetected for weeks. By the time testing became somewhat more available, community spread was already rampant in many places, making it difficult or impossible to do contact tracing and isolate people before they infected others. “In this pandemic, things moved so quickly that when you screwed up for two or three weeks, it made a difference,” Perlman says.
Testing availability has improved but remains uneven. Some experts have argued for the use of widespread rapid antigen testing, a type that is cheap, does not require sophisticated laboratory processing and could be done at homes, schools or offices. But some scientists still have concerns about the accuracy of these tests, and the FDA has been slow to approve them.
Inadequate tracing, isolating and quarantines. The timeworn methods of combatting an infectious disease—testing people who may be sick, tracing their contacts, and isolating or quarantining those who are positive or exposed—worked for COVID as well. The WHO repeatedly stressed the importance of these measures, and countries that followed this advice closely (such as Vietnam, Thailand, New Zealand and South Korea) succeeded in controlling their outbreaks. In addition to its test problems, the U.S. did not do an adequate job of isolating those who were known or suspected to be infected (or had recently traveled to a high-risk area), tracing their contacts or requiring quarantines for those who were exposed. China imposed extremely strict, city-wide quarantines. Other countries required those who may have been exposed to stay at a government-approved hotel or other facility for a quarantine ranging from a few days to a couple of weeks. Such policies would likely have been harder to implement in the U.S., a nation that prides itself on personal freedoms. But not doing so came at the expense of keeping the virus in check.
Confusing mask guidance. Although face masks are now widely considered a crucial part of stopping transmission, U.S. and global health authorities were slow to recommend them for public use. Many countries in East and Southeast Asia, including China and Japan, had normalized mask wearing well before the pandemic—in part because of the SARS outbreak in 2002–2003. Unlike the SARS virus, however, scientists now know that SARS-CoV-2 often spreads before a carrier develops symptoms (and possibly even if they never do). In the early weeks and months of the COVID outbreak, the CDC and WHO stated that face masks were not necessary for the general public unless a person was experiencing symptoms or caring for someone who was. The agencies also initially urged people not to buy high-filtration N95 and surgical masks because they were needed for health care workers and were in short supply because of inadequate government stockpiles. Though perhaps well-meaning, the WHO’s and CDC’s guidances sent a mixed message about masks’ effectiveness—and about who deserves protection. The CDC changed course and recommended cloth face coverings in April. The WHO did not do so until June, citing inadequate evidence of their efficacy before then. The CDC did not respond to a request for comment, and the WHO referred Scientific American to press briefings that addressed these issues. In these briefings, experts pointed to a lack of high-quality evidence for mask use. The WHO’s director general also stated that, in the absence of other public health measures, “masks alone will not protect you from COVID-19.”
Even after health experts reached a consensus that masks were effective, Trump refused to set an example by wearing one in public. Instead he mocked people who wore them, and many of his supporters rejected masks as well. “I don’t think it should ever become a political issue,” Rivers says. “It’s a straightforward public health intervention.” A study in Nature Medicine published online in October estimated that universal mask wearing could have saved nearly 130,000 lives during the fall and winter of 2020–2021. Most states did ultimately institute mask requirements, and Biden has made them mandatory in government buildings and on interstate transit. Yet several states, such as Texas and Mississippi, have just removed mask mandates and other restrictions entirely. “We’ve seen this happen over and over again: Where the virus picks back up, they implement more restrictions in various states and localities. It goes down a little bit, and then they just open back up again rather than saying, ‘Hey, you know, maybe this became a huge problem in the first place because we opened back up,’” Rasmussen says. “We haven’t seemed to learn from our mistakes.”
Airborne spread and “hygiene theater.” Early in the pandemic, U.S. health authorities believed the virus spread primarily by direct contact or relatively large droplets from a nearby cough or sneeze—not by far smaller droplets, called aerosols, that linger in the air. As a result, officials placed a huge emphasis on washing one’s hands and cleaning surfaces. Scientists now believe transmission from surfaces is not the main way the virus spreads and that aerosols play a much larger role. Ensuring proper ventilation and wearing well-fitted, high-quality masks are much more effective ways to reduce transmission than deep cleaning surfaces. Yet the latter—which critics have dubbed “hygiene theater”—continues to be a focus of many offices and businesses.
Structural racism fueled health inequities. The pandemic exposed and exacerbated deep-rooted racial and economic inequities in health and health care. Black and Hispanic individuals and other people of color were sickened with, and died of, COVID at disproportionately high rates. Many people in Black and brown communities had already long suffered from high rates of underlying conditions such as obesity and diabetes as a result of inadequate health care, lack of access to nutritious foods and outdoor space, and higher exposure to pollution. They also comprise a large percentage of essential workers in frontline industries with an inherently high risk of COVID exposure, such as nursing homes, meatpacking plants and restaurant kitchens. The uneven death toll is a wake-up call that far too many people of color lack access to preventative health care, as well as protections such as paid sick leave or hazard pay. “I do think the pandemic has laid bare some of those inequalities,” Rivers says. Public health experts have been tackling this problem for a long time, she notes, adding, “we need to draw on these lessons about underlying vulnerabilities from other disciplines that have such a deep understanding of how communities are affected and how to engage effectively with hard-to-reach communities.”
Decentralized response. The U.S. government’s structure meant that much of the pandemic response was left up to state and local leaders. In the absence of a strong national strategy, states implemented a patchwork of largely uncoordinated policies that did not effectively suppress the spread of the virus. This caused sudden, massive spikes of infections in many local outbreaks, placing enormous strain on health care systems and leaving no region untouched by the disease. “Every district, every county, every state could make decisions and keep them to themselves,” Gandhi says. “And we just have uneven applications of public health recommendations in a way that I can’t imagine any other country does. The Trump administration has been widely criticized for how the pandemic played out here. But Gandhi adds that the U.S. government’s decentralized nature would likely have been an obstacle under any president.
What Went Well
Despite the many mistakes and bad policy choices in the U.S. response, there were some incredible success stories, too.
Vaccines. Perhaps the clearest success amid this crisis has been the development of several vaccines in record time. Less than a year after the virus was genetically sequenced, two vaccines—one made by Pfizer and BioNTech and another developed by Moderna—were found to have roughly 95 percent efficacy in preventing symptomatic COVID and were authorized for emergency use in the U.S. The Johnson & Johnson vaccine, with efficacies of 66 percent in preventing moderate to severe disease and 85 percent in preventing severe illness alone, was recently authorized as well. (The Johnson & Johnson vaccine’s efficacy cannot be directly compared with that of the Pfizer or Moderna vaccines because the former was tested in a different population at a time when more dangerous variants of the virus were circulating.) All three vaccines prevent severe disease, hospitalization and death. “We are in an incredible place, with this pandemic, to have developed vaccines this quickly and that are that effective,” Gandhi says. Public-private partnerships were a big part of that success, she adds. Several other vaccines have been authorized or approved in other countries, and more are in development.
But the remarkable success in creating vaccines is tempered by the fact that most of the world still lacks access to them. And early rollout efforts in the U.S. had a slow and stumbling start, largely because the federal government did not provide states with the resources for distributing the vaccines. Further, Black and Hispanic people are being vaccinated at far lower rates than white people. And more work is needed to overcome vaccine hesitancy in some populations, including Republican voters. Yet the pace of vaccinations is picking up, and Biden has said the country is on track to have enough vaccine doses for every U.S. adult by the end of May, fueling promise of a return to some normality in the coming months.
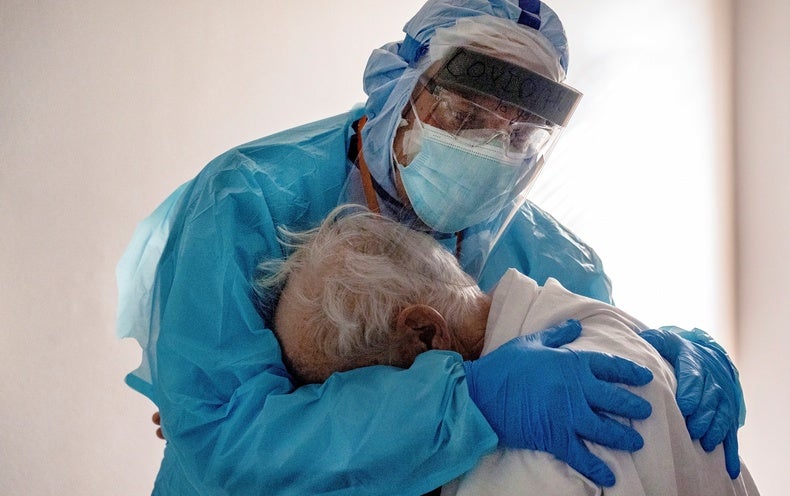
Heroic efforts of health care workers. Faced with unprecedented levels of sickness and death, health care workers stepped up and risked their lives to care for COVID patients. Nurses, aides and orderlies cared for the elderly and most vulnerable individuals as the virus ravaged nursing homes. Paramedics responded to calls at all hours of the night. Doctors, nurses and other hospital staff comforted dying patients as they struggled to breathe—and held their hand when they said goodbye over video calls to family members who were not allowed in the room with them. Over time, medical professionals learned better techniques for treating the disease: these ranged from pharmaceuticals such as steroids and monoclonal antibodies to low-tech interventions, including “proning,” or simply turning some patients onto their stomach so they can breathe more easily. Even as nursing homes and hospitals became overwhelmed with COVID patients, hardworking staff kept showing up, shift after shift, facing down terror, exhaustion and despair.
The public (mostly) did its part. Despite COVID becoming a part of the country’s bitter and escalating political divide, many Americans followed public health guidance regarding mask wearing, social distancing and avoiding unnecessary risks. Surveys show the majority of people wear masks when they go out, Johns Hopkins’s Rivers says. “I am really heartened by the sense of purpose—the willingness for the whole country to come together and change their lives and protect themselves and their communities,” she says.
Combatting misinformation. In a media environment where misinformation and disinformation can reach millions through a single tweet, sorting out the signal from the noise has been an enormous challenge. But for the most part, science journalists confronted the informational chaos with clear, evidence-based reporting. When Trump made unsupported claims about safety levels or mask wearing or dubious COVID “treatments,” journalists and high-profile scientists such as Anthony Fauci quickly set the record straight. But as conspiracy theorists continue to circulate misinformation about the disease and vaccines, it is more important than ever that media outlets remain on guard.
Lingering Questions
As the world passes this one-year milestone in the pandemic, many unknowns remain.
What will happen with the new variants? Several novel strains of SARS-CoV-2 have emerged that could threaten progress against the disease. A variant called B.1.1.7, first identified in the U.K., is deadlier and more transmissible than the original—and it is on track to become the dominant variant in the U.S. this spring. Another variant that was initially spotted in South Africa, called B.1.351, has mutations that appear to help it to at least partially evade some of the vaccines. A third variant that was first seen in Brazil, called P.1, has overrun parts of that country and also contains worrisome mutations. Currently these variants are in a race with the vaccines, and scientists hope enough people can be vaccinated quickly enough to outmaneuver the new strains. Some vaccine makers are already working on booster shots, should they be necessary.
How long will immunity last? The duration of immunity to COVID—whether from natural infection or vaccination—remains unknown. A large study demonstrated that people who had recovered from infection still had antibodies, as well as so-called memory B cells and memory T cells, six to eight months later. A number of reinfections have occurred with some of the new variants, however. The CDC recently released guidelines stating that, with a few exceptions, fully vaccinated people who are exposed to the virus do not need to quarantine if they do not show symptoms. Time will tell whether vaccination provides immunity that lasts months or years and if booster shots will be needed.
Why do some people become COVID “long haulers”? A certain percentage of people who get COVID develop lingering symptoms that persist for months after their initial infection. Symptoms range from extreme fatigue to brain fog to problems sleeping. Scientists do not yet fully understand why some individuals experience these disturbing effects, although other viral infections have been known to produce similar syndromes. The National Institutes of Health has announced plans to invest $1 billion to study “long COVID.” But the illness’s true impact on people’s lives may not be known for decades.
What is the future of SARS-CoV-2? Exactly what will happen to the virus over time remains a mystery. Most scientists think it will never go away completely but could become less common and milder as more people are vaccinated against it—or as they build up some immunity through natural infection. It may ultimately become something like the flu, a virus that circulates every year and causes some severe infections and deaths—but does not shut down society. Eventually it could evolve into a less virulent form like some strains of the common cold. But that could take many years.
Read more about the coronavirus outbreak from Scientific American here. And read coverage from our international network of magazines here.

